Bilateral Hallux Valgus Deformities
Overview
 A bunion is a firm, painful bump that forms over a bony bulge at the base of the big toe. In most cases, the big toe joint also is enlarged and has degenerative arthritis. The toe also may be pushed toward the second toe (hallux valgus). Bunions tend to be inherited, but they also are common in the following groups. Women who wear high heels. People who wear shoes that are too narrow or too pointed. People with flatfeet. All of these situations force the big toe to drift toward the little toes, and this can cause bunions to form.
A bunion is a firm, painful bump that forms over a bony bulge at the base of the big toe. In most cases, the big toe joint also is enlarged and has degenerative arthritis. The toe also may be pushed toward the second toe (hallux valgus). Bunions tend to be inherited, but they also are common in the following groups. Women who wear high heels. People who wear shoes that are too narrow or too pointed. People with flatfeet. All of these situations force the big toe to drift toward the little toes, and this can cause bunions to form.
Causes
Bunions are a common problem experienced mostly by women. The deformity can develop from an abnormality in foot function, or arthritis, but is more commonly caused by wearing improper fitting footwear. Tight, narrow dress shoes with a constrictive toe box (toe area) can cause the foot to begin to take the shape of the shoe, leading to the formation of a bunion. Women who have bunions normally wear dress shoes that are too small for their feet. Their toes are squeezed together in their shoes causing the first metatarsal bone to protrude on the side of the foot. It is important for men and women to realize that wearing dress shoes and boots, which are tapered in the toe area, can cause the bunion to worsen to the point where surgery is necessary.
Symptoms
While bunions may be considered cosmetically undesirable, they are not necessarily painful. In cases where the individual has minor discomfort that can be eased by wearing wider shoes made of soft leather and/or with the aid of spacers-padding placed between the toes to correct alignment-further treatment may not be necessary. (Anti-inflammatory agents can be used to alleviate temporary discomfort at the site of the bursa.) For those who continue to experience pain on a daily basis and who cannot wear most types of shoe comfortably, surgical treatment may be the best choice.
Diagnosis
Most patients are diagnosed to have bunions from clinical history and examination. However, in some cases, X-rays will be performed to determine the extent of damage to the joint. Furthermore, it will enable the treating doctor to decide on the best course of management of the patient.
Non Surgical Treatment
Apply special pads and dressings to protect the bunion from shoe pressure. Inject steroid and local anesthetic around the bunion to reduce inflammation. This is especially useful if there is an associated bursitis. Recommend commercially available or custom made shoes. Prescribe functional orthotics to correct faulty foot function, and help prevent worsening of the deformity. Recommend bunion surgery to correct the deformity. 
Surgical Treatment
Several surgical procedures are available to the podiatric physician The surgery will remove the bony enlargement, restore the normal alignment of the toe joint, and relieve pain.A simple bunionectomy, in which only the bony prominence is removed, may be used for the less severe deformity. Severe bunions may require a more involved procedure, which includes cutting the bone and realigning the joint. Recuperation takes time, and swelling and some discomfort are common for several weeks following surgery. Pain, however, is easily managed with medications prescribed by your podiatric physician.
Prevention
Here are some tips to help you prevent bunions. Wear shoes that fit well. Use custom orthotic devices. Avoid shoes with small toe boxes and high heels. Exercise daily to keep the muscles of your feet and legs strong and healthy. Follow your doctor?s treatment and recovery instructions thoroughly. Unfortunately, if you suffer from bunions due to genetics, there may be nothing you can do to prevent them from occurring. Talk with your doctor about additional prevention steps you can take, especially if you are prone to them.
Overpronation Of The Foot
Over-pronation occurs when the foot collapses too far inward stressing the plantar fascia (the area underneath the arch of the foot.) Normally, one pronates every time he/she walks, but excessive pronation is called over-pronation. When this occurs it can cause pain in the feet, knees, hips, low back and even the shoulder.

Causes
There are many biomechanical issues that can contribute to excessive pronation, including weak foot intrinsic muscles, limited ankle dorsiflexion mobility and calf flexibility, weak ankle invertor muscles (e.g. posterior tibialis), weak forefoot evertor muscles (peroneus longus), poor hip strength and control, Anterior pelvic tilting, heel InversionIn a person who overpronates, the heel bone goes into an everted position meaning that it turns out away from the midline of the body. The opposite motion of eversion is inversion. Inversion is a motion that needs to be controlled to prevent the foot from excessively pronating.
Symptoms
If you overpronate, your symptoms may include discomfort in the arch and sole of foot. Your foot may appear to turn outward at the ankle. Your shoes wear down faster on the medial (inner) side of your shoes. Pain in ankle, shins, knees, or hips, especially when walking or running.Unfortunately, overpronation can lead to additional problems with your feet, ankles, and knees. Runners in particular find that overpronation can lead to shin splints, tarsal tunnel syndrome, plantar fasciitis, compartment syndrome, achilles tendonitis, bunions (hallux valgus) patello femoral pain syndrome, heel spurs, metatarsalgia. You do not have to be a runner or athlete to suffer from overpronation. Flat feet can be inherited, and many people suffer from pain on a day-to-day basis. Flat feet can also be traumatic in nature and result from tendon damage over time. Wearing shoes that do not offer enough arch support can also contribute to overpronation.
Diagnosis
If you cannot afford to get a proper gait analysis completed, having someone observe you on a treadmill from behind will give you an idea if you are an overpronator. It is possible to tell without observing directly whether you are likely to be an overpronator by looking at your foot arches. Check your foot arch height by standing in water and then on a wet floor or piece of paper which will show your footprint. If your footprints show little to no narrowing in the middle, then you have flat feet or fallen arches. This makes it highly likely that you will overpronate to some degree when running. If you have low or fallen arches, you should get your gait checked to see how much you overpronate, and whether you need to take steps to reduce the level to which you overpronate. Another good test is to have a look at the wear pattern on an old pair of trainers. Overpronators will wear out the outside of the heel and the inside of the toe more quickly than other parts of the shoe. If the wear is quite even, you are likely to have a neutral running gait. Wear primarily down the outside edge means that you are a supinator. When you replace your running shoes you may benefit from shoes for overpronation. Motion control or stability running shoes are usually the best bet to deal with overpronation.

Non Surgical Treatment
Supportive orthotics in the shoe is a method commonly implemented to treat many common running injuries associated with pronation. An advantage of orthotics is that they often allow the sufferer to continue to participate in athletic activity and avoid other treatment options that could be potentially costly and time consuming. Seventy-five percent of injured runners are successfully treated with the prescription of orthoses. Orthotics are the most effective treatment for symptoms that develop from unusual biomechanics within the body such as overpronation, resulting in either great improvement or complete healing of the injury in about half the cases.
Prevention
Many of the prevention methods for overpronation-orthotics, for example-can be used interchangeably with treatment methods. If the overpronation is severe, you should seek medical attention from a podiatrist who can cast you for custom-made orthotics. Custom-made orthotics are more expensive, but they last longer and provide support, stability, and balance for the entire foot. You can also talk with a shoe specialist about running shoes that offer extra medial support and firm heel counters. Proper shoes can improve symptoms quickly and prevent them from recurring. Surgery can sometimes help cure and prevent this problem if you suffer from inherited or acquired pes planus deformity. Surgery typically involves stabilizing the bones to improve the foot?s support and function.
Severs Disease Physiotherapy
Sever?s disease is the most common cause of heel pain in the growing athlete and is due to overuse and repetitive microtrauma of growth plates in the heel. It occurs in children ages 7 to 15, with the majority of patients presenting between 10 and 14 years of age. Sever?s disease will go away on its own when it is used less or when the bone is through growing, but it can recur (for example, at the start of a new sports season). Traditionally, the only known cure was for children to outgrow the condition, with recurrences happening an average of 18 months before this occurs.
Causes
Sever's Disease is a repetitive strain injury caused by the following. High impact injury activities and sport like netball, football, soccer, hockey, basketball, running, jumping and tennis. Tight calf muscles. Poor mechanics, structure and function of the foot. Excessive pronation. Rapid growth spurt. The above causes tension, inflammation and pain where the Achilles tendon inserts onto the calcaneus (Back/bottom surface of the heel bone). It is important that this problem is treated and monitored until the growth plate ossifies in the heel. This could occur between the ages of 14 and 16 years of age. In extreme cases the growth plate can become separated from the calcaneus.
Symptoms
Symptoms include Heel Pain. Pain at the back of the heels when walking or running. Possibly a lump at the back of the heel, although this might be minimal. Pain and tenderness at the back of the heels, especially if you press on it, or give it a squeeze from the sides. Tight calf muscles resulting in reduced ankle range of motion.
Diagnosis
Sever's disease is diagnosed based on a doctor?s physical examination of the lower leg, ankle, and foot. If the diagnosis is in question, the doctor may order X-rays or an MRI to determine if there are other injuries that may be causing the heel pain.
Non Surgical Treatment
The following are different treatment options Rest and modify activity. Limit running and high-impact activity to rest the heel and lessen the pain. Choose one running or jumping sport to play at a time. Substitute low-impact cross-training activities to maintain cardiovascular fitness. This can include biking, swimming, using a stair-climber or elliptical machine, rowing, or inline skating. Reduce inflammation. Ice for at least 20 minutes after activity or when pain increases. Nonsteroidal anti-inflammatory drugs (NSAIDs) may also help. Stretch the calf. Increase calf flexibility by doing calf stretches for 30 to 45 seconds several times per day. Protect the heel. The shoe may need to be modified to provide the proper heel lift or arch support. Select a shoe with good arch support and heel lift if possible. Try heel lifts or heel cups in sports shoes, especially cleats. Try arch support in cleats if flat feet contribute to the problem. Take it one step at a time. Gradually resume running and impact activities as symptoms allow. Sever?s disease usually goes away when the growth plate (apophysis) matures, which should be by age 12 to 13 years in females and 13 to 14 years in males.
Recovery
Although Sever's disease generally heals quickly, it can recur if long-term measures are not taken to protect the heel during a child's growing years. One of the most important is to make sure that kids wear proper shoes. Good quality, well-fitting shoes with shock-absorbent (padded) soles help to reduce pressure on the heel. The doctor may also recommend shoes with open backs, such as sandals or clogs, that do not rub on the back of the heel. Shoes that are heavy or have high heels should be avoided. Other preventive measures include continued stretching exercises and icing of the affected heel after activity.
Surgery For Flat Feet In Adults
Overview
Adult-acquired flatfoot is a challenging condition to treat. It is defined as a symptomatic, progressive deformity of the foot caused by loss of supportive structures of the medial arch. It is becoming increasingly frequent with the aging population and the obesity epidemic. Patients commonly try to lose weight by exercising to improve the condition. This often leads to worsening of symptoms and progression of the disorder. Early recognition of this complex disorder is essential, if chronic pain and surgery are to be avoided. 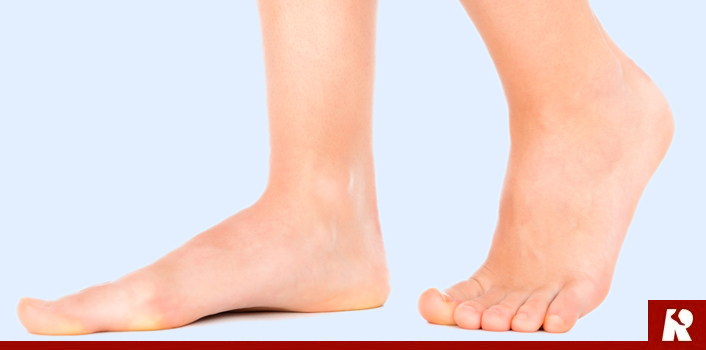
Causes
Obesity - Overtime if your body is carrying those extra pounds, you can potentially injure your feet. The extra weight puts pressure on the ligaments that support your feet. Also being over weight can lead to type two diabetes which also can attribute to AAFD. Diabetes - Diabetes can also play a role in Adult Acquired Flatfoot Deformity. Diabetes can cause damage to ligaments, which support your feet and other bones in your body. In addition to damaged ligaments, uncontrolled diabetes can lead to ulcers on your feet. When the arches fall in the feet, the front of the foot is wider, and outer aspects of the foot can start to rub in your shoe wear. Patients with uncontrolled diabetes may not notice or have symptoms of pain due to nerve damage. Diabetic patient don?t see they have a problem, and other complications occur in the feet such as ulcers and wounds. Hypertension - High blood pressure cause arteries narrow overtime, which could decrease blood flow to ligaments. The blood flow to the ligaments is what keeps the foot arches healthy, and supportive. Arthritis - Arthritis can form in an old injury overtime this can lead to flatfeet as well. Arthritis is painful as well which contributes to the increased pain of AAFD. Injury - Injuries are a common reason as well for AAFD. Stress from impact sports. Ligament damage from injury can cause the bones of the foot to fallout of ailment. Overtime the ligaments will tear and result in complete flattening of feet.
Symptoms
Pain along the inside of the foot and ankle, where the tendon lies. This may or may not be associated with swelling in the area. Pain that is worse with activity. High-intensity or high-impact activities, such as running, can be very difficult. Some patients can have trouble walking or standing for a long time. Pain on the outside of the ankle. When the foot collapses, the heel bone may shift to a new position outwards. This can put pressure on the outside ankle bone. The same type of pain is found in arthritis in the back of the foot. Asymmetrical collapsing of the medial arch on the affected side.
Diagnosis
Your podiatrist is very familiar with tendons that have just about had enough, and will likely be able to diagnose this condition by performing a physical exam of your foot. He or she will probably examine the area visually and by feel, will inquire about your medical history (including past pain or injuries), and may also observe your feet as you walk. You may also be asked to attempt standing on your toes. This may be done by having you lift your ?good? foot (the one without the complaining tendon) off the ground, standing only on your problem foot. (You may be instructed to place your hands against the wall to help with balance.) Then, your podiatrist will ask you to try to go up on your toes on the bad foot. If you have difficulty doing so, it may indicate a problem with your posterior tibial tendon. Some imaging technology may be used to diagnose this condition, although it?s more likely the doctor will rely primarily on a physical exam. However, he or she may order scans such as an MRI or CT scan to look at your foot?s interior, and X-rays might also be helpful in a diagnosis.
Non surgical Treatment
Although AAF is not reversible without surgery, appropriate treatment should address the patient?s current symptoms, attempt to reduce pain, and allow continued ambulation. In the early stages, orthotic and pedorthic solutions can address the loss of integrity of the foot?s support structures, potentially inhibiting further destruction.3-5 As a general principle, orthotic devices should only block or limit painful or destructive motion without reducing or restricting normal motion or muscle function. Consequently, the treatment must match the stage of the deformity. 
Surgical Treatment
If initial conservative therapy of posterior tibial tendon insufficiency fails, surgical treatment is considered. Operative treatment of stage 1 disease involves release of the tendon sheath, tenosynovectomy, debridement of the tendon with excision of flap tears, and repair of longitudinal tears. A short-leg walking cast is worn for 3 weeks postoperatively. Teasdall and Johnson reported complete relief of pain in 74% of 14 patients undergoing this treatment regimen for stage 1 disease. Surgical debridement of tenosynovitis in early stages is believed to possibly prevent progression of disease to later stages of dysfunction.
Heel Soreness

Heel pain can vary from moderate to severe pain that can make walking and daily tasks a chore if not treated. There are a number of different conditions which can cause Heel Pain so it is important that your heel is properly assessed and diagnosed by a Podiatrist. The most common cause of heel pain is plantar fasciitis. This is where the tissue becomes inflamed at the heel bone or along sole of the foot between the heel and toe. Another condition commonly referred to as a heel spur can also cause pain in the heel. A heel spur is when a spike of bone has been pulled away from the heel bone, where the plantar fascia inserts, causing pain in the area directly under the heel on direct pressure.
Causes
The most common cause of heel pain in adults is plantar fasciitis, which is an inflammation of the band of tissue in the sole that connects the heel to the toes and forms the natural foot arch. Plantar fasciitis may or may not be complicated by a calcaneal spur, a small bone growth that protrudes out of the heel. Plantar fasciitis may also be referred to as plantar fasciosis. In contrast to fasciitis, which essentially means inflammation, fasciosis refers to degeneration of the tissue. In fact, if left untreated, acute plantar fasciitis may develop into a chronic painful condition, which results in slow and irreversible degeneration of the fascia, hence plantar fasciosis. The location of the pain is usually exactly under the heel but may also occur in the arch of the foot. Pain typical to plantar fasciitis is that which feels worse when arising on to your feet such as in mornings or after sitting down for a while, and usually progresses in severity when left untreated.
Symptoms
Symptoms may also include swelling that is quite tender to the touch. Standing, walking and constrictive shoe wear typically aggravate symptoms. Many patients with this problem are middle-aged and may be slightly overweight. Another group of patients who suffer from this condition are young, active runners.
Diagnosis
To arrive at a diagnosis, the foot and ankle surgeon will obtain your medical history and examine your foot. Throughout this process the surgeon rules out all the possible causes for your heel pain other than plantar fasciitis. In addition, diagnostic imaging studies such as x-rays or other imaging modalities may be used to distinguish the different types of heel pain. Sometimes heel spurs are found in patients with plantar fasciitis, but these are rarely a source of pain. When they are present, the condition may be diagnosed as plantar fasciitis/heel spur syndrome.
Non Surgical Treatment
Heel pain often goes away on its own with home care. For heel pain that isn't severe, try the following. Rest. If possible, avoid activities that put stress on your heels, such as running, standing for long periods or walking on hard surfaces. Ice. Place an ice pack or bag of frozen peas on your heel for 15 to 20 minutes three times a day. New shoes. Be sure your shoes fit properly and provide plenty of support. If you're an athlete, choose shoes appropriate for your sport and replace them regularly. Foot supports. Heel cups or wedges that you buy in the drugstore often provide relief. Custom-made orthotics usually aren't needed for heel problems. Over-the-counter pain medications. Aspirin or ibuprofen (Advil, Motrin IB, others) can reduce inflammation and pain.
Surgical Treatment
Although most patients with plantar fasciitis respond to non-surgical treatment, a small percentage of patients may require surgery. If, after several months of non-surgical treatment, you continue to have heel pain, surgery will be considered. Your foot and ankle surgeon will discuss the surgical options with you and determine which approach would be most beneficial for you. No matter what kind of treatment you undergo for plantar fasciitis, the underlying causes that led to this condition may remain. Therefore, you will need to continue with preventive measures. Wearing supportive shoes, stretching, and using custom orthotic devices are the mainstay of long-term treatment for plantar fasciitis.
Prevention

Prevention of heel pain involves reducing the stress on that part of the body. Tips include. Barefeet, when on hard ground make sure you are wearing shoes. Bodyweight, if you are overweight there is more stress on the heels when you walk or run. Try to lose weight. Footwear, footwear that has material which can absorb some of the stress placed on the heel may help protect it. Examples include heel pads. Make sure your shoes fit properly and do not have worn down heels or soles. If you notice a link between a particular pair of shoes and heel pain, stop wearing them. Rest, if you are especially susceptible to heel pain, try to spend more time resting and less time on your feet. It is best to discuss this point with a specialized health care professional. Sports, warm up properly before engaging in activities that may place lots of stress on the heels. Make sure you have proper sports shoes for your task.
Achilles Tendonitis
 This nagging injury can be long-lasting if not treated - and if your running form needs some work. The name Achilles is said to be a combination of two Greek words that together mean ?grief of the people.? The injury that bears that hero?s name, in honor of his only weakness, certainly aggrieves many runners, with Achilles tendinitis accounting for around 10 percent of running injuries. Technically, Achilles tendinitis is acute inflammation of the tendon that runs along the back of the ankle. Pain in that area for longer than a couple weeks is not really tendinitis anymore. Athletes, however, tend to characterize any pain along the tendon above the back of the heel as Achilles tendinitis. Achilles tendinitis can be confused with other injuries, such as heel problems, but the hallmark sign is if you?re pinching the Achilles and it?s really sore.
This nagging injury can be long-lasting if not treated - and if your running form needs some work. The name Achilles is said to be a combination of two Greek words that together mean ?grief of the people.? The injury that bears that hero?s name, in honor of his only weakness, certainly aggrieves many runners, with Achilles tendinitis accounting for around 10 percent of running injuries. Technically, Achilles tendinitis is acute inflammation of the tendon that runs along the back of the ankle. Pain in that area for longer than a couple weeks is not really tendinitis anymore. Athletes, however, tend to characterize any pain along the tendon above the back of the heel as Achilles tendinitis. Achilles tendinitis can be confused with other injuries, such as heel problems, but the hallmark sign is if you?re pinching the Achilles and it?s really sore.
Causes
There are several factors that can contribute to achilles tendonitis. First, you should know that the biggest contributor to chronic achilles tendonitis is ignoring pain in your achilles tendon and running through the pain of early achilles tendonitis. If your achilles tendon is getting sore it is time to pay attention to it, immediately. Sudden increases in training can contribute to achilles tendonitis. Excessive hill running or a sudden addition of hills and speed work can also contribute to this problem. Two sole construction flaws can also aggravate achilles tendonitis. The first is a sole that is too stiff, especially at the ball of the foot. (In case you are having difficulty locating the "ball" of your foot, I mean the part where the toes join the foot and at which the foot bends) If this area is stiff than the "lever arm" of the foot is longer and the achilles tendon will be under increased tension and the calf muscles must work harder to lift the heel off the ground. The second contributing shoe design factor which may lead to continuing achilles tendon problem is excessive heel cushioning. Air filled heels, while supposedly are now more resistant to deformation and leaks are not good for a sore achilles tendon. The reason for this is quite simple. If you are wearing a shoe that is designed to give great heel shock absorption what frequently happens is that after heel contact, the heel continues to sink lower while the shoe is absorbing the shock. This further stretches the achilles tendon, at a time when the leg and body are moving forward over the foot. Change your shoes to one without this "feature". Of course another major factor is excessive tightness of the posterior leg muscles, the calf muscles and the hamstrings may contribute to prolonged achilles tendonitis. Gentle calf stretching should be performed preventatively. During a bout of acute achilles tendonitis, however, overly exuberant stretching should not be performed.
Symptoms
The pain associated with Achilles tendinitis typically begins as a mild ache in the back of the leg or above the heel after running or other sports activity. Episodes of more severe pain may occur after prolonged running, stair climbing or sprinting. You might also experience tenderness or stiffness, especially in the morning, which usually improves with mild activity. If you experience persistent pain around the Achilles tendon, call your doctor. Seek immediate medical attention if the pain or disability is severe. You may have a torn (ruptured) Achilles tendon.
Diagnosis
Physicians usually pinch your Achilles tendon with their fingers to test for swelling and pain. If the tendon itself is inflamed, your physician may be able to feel warmth and swelling around the tissue, or, in chronic cases, lumps of scar tissue. You will probably be asked to walk around the exam room so your physician can examine your stride. To check for complete rupture of the tendon, your physician may perform the Thompson test. Your physician squeezes your calf; if your Achilles is not torn, the foot will point downward. If your Achilles is torn, the foot will remain in the same position. Should your physician require a closer look, these imaging tests may be performed. X-rays taken from different angles may be used to rule out other problems, such as ankle fractures. MRI (magnetic resonance imaging) uses magnetic waves to create pictures of your ankle that let physicians more clearly look at the tendons surrounding your ankle joint.
Nonsurgical Treatment
Most cases are successfully treated non-surgically although this is time-consuming and frustrating for active patients. Treatment is less likely to be successful if symptoms have been present more than six months. Nonsurgical management includes nonsteroidal anti-inflammatory medications, rest, immobilization, limitation of activity, ice, contrast baths, stretching and heel lifts. If symptoms fail to resolve after two to three months, a formal physical therapy program may be of benefit. An arch support may help if there is an associated flatfoot. A cast or brace to completely rest this area may be necessary. Extracorporeal shockwave therapy and platelet-rich plasma injections? have variable reports of success. Nitroglycerin medication applied to the overlying skin may be of benefit.
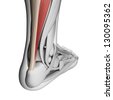
Surgical Treatment
Achilles tendon repair surgery is often used to repair a ruptured or torn Achilles tendon, the strong fibrous cord that connects the two large muscles in the back of your calf to your heel bone. These muscles (the gastrocnemius and the soleus) create the power needed to push off with your foot or rise up on your toes. Achilles tendon ruptures are quite common. Most happen during recreational activities that require sudden bursts of muscle power in the legs. Often a torn Achilles tendon can be diagnosed with a physical examination. If swelling is present, the orthopaedist may delay the Achilles tendon surgery until it subsides.
Prevention
Appropriately warm up and stretch before practice or competition. Allow time for adequate rest and recovery between practices and competition. Maintain appropriate conditioning, Ankle and leg flexibility, Muscle strength and endurance, Cardiovascular fitness. Use proper technique. To help prevent recurrence, taping, protective strapping, or an adhesive bandage may be recommended for several weeks after healing is complete.
What Is Plantar Fasciitis

Overview
Plantar fasciitis is a dull to severe pain in your heel caused by a strain and inflammation of your plantar fascia. The plantar fascia is a scientific name for “foot tissue”. This particular tissue is a ligament attached at one side to the heel bone. At the other side, the tissue fans out to attach at the base of each of your five toes. Plantar fasciitis is the name for the condition that develops when that tissue becomes inflamed. When the plantar fascia is excessively stretched, micro-tears can occur, causing this swelling and subsequent pain.
Causes
When the foot moves, the plantar fascia stretches and contracts. Plantar fasciitis is caused by the repetitive overstretching of the plantar fascia. If the tension on the plantar fascia is too great, this overstretching causes small tears in the plantar fascia. This in turn causes the plantar fascia to become inflamed and painful. Factors that contribute to the development of plantar fasciitis include having very high arches or flat feet, gender, while anyone can develop plantar fasciitis, it tends to occur more commonly in women, exercises such as running, walking and dancing, particularly if the calf muscles are tight. Activities or occupations that involve walking or standing for long periods of time, particularly on hard surfaces, wearing high heeled shoes or shoes that do not offer adequate arch support and cushioning, being overweight, additional weight increases the tension on the plantar fascia, poor biomechanics, extra tension is placed on the plantar fascia if weight is not spread evenly when standing, walking or running. Some cases of plantar fasciitis may be linked to underlying diseases that cause arthritis, such as ankylosing spondylitis.
Symptoms
You'll typically first notice early plantar fasciitis pain under your heel or in your foot arch in the morning or after resting. Your heel pain will be worse with the first steps and improves with activity as it warms up. As plantar fasciitis deteriorates, the pain will be present more often. You can determine what stage your are in using the following guidelines. No Heel Pain, Normal! Heel pain after exercise. Heel pain before and after exercise. Heel pain before, during and after exercise. Heel pain all the time. Including at rest! This symptom progression is consistent with the four stages of a typical overuse injury. Ultimately, further trauma and delayed healing will result in the formation of calcium (bone) within the plantar fascia. When this occurs adjacent to the heel bone it is known as heel spurs, which have a longer rehabilitation period.
Diagnosis
Your doctor will check your feet and watch you stand and walk. He or she will also ask questions about your past health, including what illnesses or injuries you have had. Your symptoms, such as where the pain is and what time of day your foot hurts most. How active you are and what types of physical activity you do. Your doctor may take an X-ray of your foot if he or she suspects a problem with the bones of your foot, such as a stress fracture.
Non Surgical Treatment
The key for the proper treatment of plantar fasciitis is determining what is causing the excessive stretching of the plantar fascia. When the cause is over-pronation (flat feet), an orthotic with rearfoot posting and longitudinal arch support is an effective device to reduce the over-pronation and allow the condition to heal. If you have usually high arches, which can also lead to plantar fasciitis, cushion the heel, absorb shock and wear proper footwear that will accommodate and comfort the foot. Other common treatments include stretching exercises, plantar fasciitis night splints, wearing shoes that have a cushioned heel to absorb shock, and elevating the heel with the use of a heel cradle or heel cup. Heel cradles and heel cups provide extra comfort, cushion the heel, and reduce the amount of shock and shear forces placed during everyday activities.

Surgical Treatment
The most common surgical procedure for plantar fasciitis is plantar fascia release. It involves surgical removal of a part from the plantar fascia ligament which will relieve the inflammation and reduce the tension. Plantar fascia release is either an open surgery or endoscopic surgery (insertion of special surgical instruments through small incisions). While both methods are performed under local anesthesia the open procedure may take more time to recover. Other surgical procedures can be used as well but they are rarely an option. Complications of plantar fasciitis surgery are rare but they are not impossible. All types of plantar fasciitis surgery pose a risk of infection, nerve damage, and anesthesia related complications including systemic toxicity, and persistence or worsening of heel pain.
Prevention
Being overweight can place excess pressure and strain on your feet, particularly on your heels. Losing weight, and maintaining a healthy weight by combining regular exercise with a healthy, balanced diet, can be beneficial for your feet. Wearing appropriate footwear is also important. Ideally, you should wear shoes with a low to moderate heel that supports and cushions your arches and heels. Avoid wearing shoes with no heels.